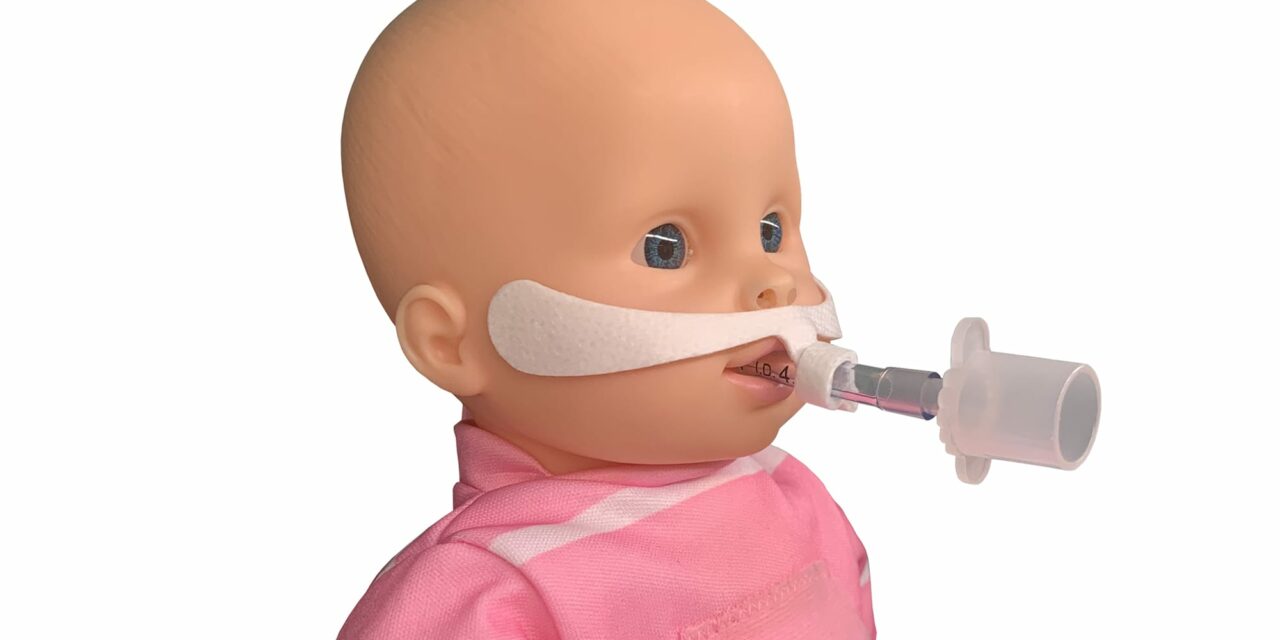
Endotracheal tube fixation has to remain stable through routine care events, moisture exposure, oral care, and changing sedation levels. When securement drifts, even slightly, clinicians can see it show up as changing leak behavior, inconsistent ventilation, new pressure points, or a tube position that no longer matches the documented depth. A stable approach protects the airway plan by keeping the position consistent while still allowing suctioning, turns, and hygiene without repeated rework.
In practice, performance comes from both the device and the method. With Et Tube Securement Devices, clinicians look at facial anatomy, adhesive behavior in humidity, circuit pull direction, and how quickly a setup can be reassessed during the shift. Securement is treated as ongoing airway management, with quick checks that prevent small movements from becoming a bigger problem.
Clinical Use Cases for Et Tube Securement Devices in Anesthesia and ICU Care
Securement devices are used to maintain tube position and reduce unintended movement during anesthesia, transport, and intensive care monitoring. They become especially important when repeated handling is expected, including suctioning, repositioning, and oral hygiene, because stable fixation reduces the need to re-tape and re-measure during care events. That stability also supports clearer trend interpretation, since ventilation changes are less likely to be caused by tube movement.
Clinicians also consider how securement holds as sedation changes. When a patient becomes more responsive, jaw movement, coughing, and bite force can increase stress on fixation points. In these moments, securement has to hold without increasing soft tissue trauma, which is why clinicians balance stability with skin and mucosal tolerance.
Bedside Checks That Confirm ET Tube Securement and Reduce Drift
After placement, clinicians confirm the documented depth marking, symmetry at the lip line, and the direction of pull created by the ventilator circuit. They also check whether the adhesive surface area matches the patient’s skin condition and whether moisture is likely to compromise hold during the shift. The most useful checks are the ones that can be repeated quickly and consistently, especially after turns, transport, or high secretion periods.
Ongoing evaluation includes watching for pressure points, edge lift, and early skin irritation, then correcting small problems before fixation fails. When facial skin is delicate, or if the patient is sweating profusely, clinicians modify their approach to ensure the tube stays put while minimizing the likelihood of skin damage. For a more in-depth understanding of securement principles and the factors that influence clinical decisions, read Endotracheal Securement.
Design Features That Improve Stability and Protect Skin Tolerance
Securement performance is influenced by how the device distributes load across the face, how it resists peel forces, and how it handles moisture at the adhesive interface. Clinicians often prefer designs that keep fixation predictable during routine care, because every rework adds time, discomfort, and incremental skin trauma. A stable design also reduces the likelihood of repeated adhesive removal in a short window, which is a common driver of irritation.
Device choice also affects workflow across a shift. A design that supports quick reassessment, predictable repositioning habits, and stable circuit routing makes it easier to maintain position without disrupting ventilation. For a broader discussion of how airway fixation supports patient safety in high acuity environments, read Endotracheal Tube Holders: Enhancing Patient Safety in Anesthesia & Intensive Care for a detailed understanding.
B&B Medical Technologies Support for Airway Securement Workflows
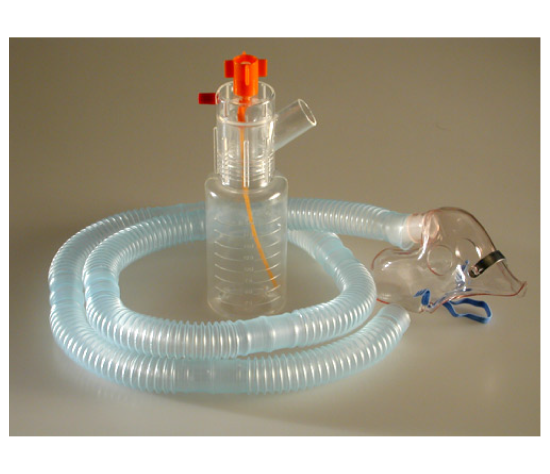
B&B Medical Technologies develops airway and respiratory care products used in environments where securement has to remain reliable through repeated bedside care. That long-standing focus informs designs that support consistent application, predictable hold in humidity, and fast reassessment during routine events such as oral care, repositioning, and circuit management. Products are built around practical clinical routines where small adjustments need to be made without losing the airway plan, reflecting an understanding of foundational concepts like the Bubble CPAP Working Principle, where stability and controlled pressure delivery are essential to effective respiratory support.
By prioritizing repeatable use and stable performance, B&B Medical Technologies helps clinicians maintain fixation that stays consistent without adding unnecessary complexity. With Et Tube Securement Devices, this translates into securement that is easier to standardize across shifts, easier to check after handling, and more predictable to troubleshoot when conditions change. When securement remains reliable and easy to assess, clinicians can stay focused on ventilation goals, patient response, and skin protection while maintaining confidence in tube position—aligned with the same consistency-driven approach seen in the Bubble CPAP Working Principle, where dependable system behavior supports clearer clinical decision-making.
Frequently Asked Questions
Devices can provide more consistent fixation and reduce repeated re-taping during routine care. They also support faster reassessment when patient condition or handling changes.
Clinicians confirm tube depth marking, alignment at the lip line, circuit pull direction, and early skin pressure points. These checks help catch drift before it becomes a ventilation or safety issue.
Moisture can weaken adhesion and increase edge lift, especially with sweating or oral secretions. Securement plans often account for skin prep and predictable rechecks.
Adjustment is considered when fixation loosens, skin irritation develops, or tube position changes. Clinicians also reassess after major handling events like turns or transport.
Stable securement supports consistent ventilation and reduces unintended movement that can affect airway protection. It also helps maintain predictable care routines during high-acuity monitoring.