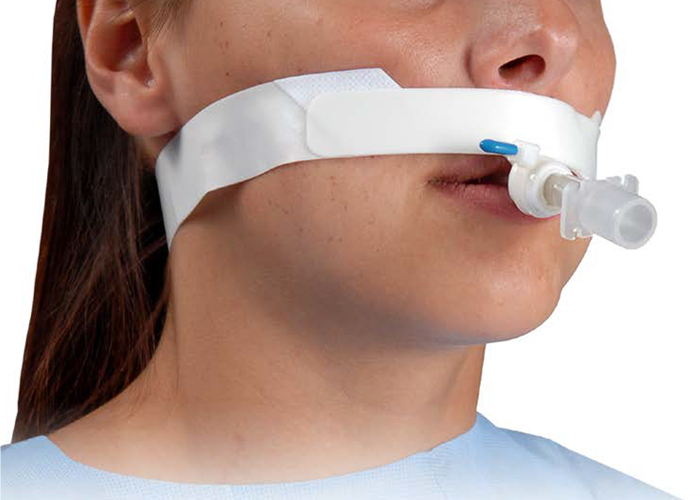
Airway protection does not end once an endotracheal tube is placed. In ventilated patients, the next challenge is preserving tube patency and position while the patient moves through sedation changes, agitation, oral reflex activity, and routine care. Biting introduces a form of airway risk that can develop suddenly because the pressure is applied directly to the tube at the point where airflow is already most vulnerable to compression. Once that pressure narrows the lumen, ventilation becomes less reliable, airway resistance rises, and the patient can deteriorate quickly if the problem is not recognized and corrected.
That is where Bite Blocks become part of airway protection rather than a secondary add-on. Their purpose is not limited to preventing visible tube damage. They help preserve a clear airflow path, reduce the risk of bite-related obstruction, and support more consistent ventilation under conditions where patient response can change from one moment to the next. When they are used alongside stable securement with an Endotracheal Tube Holder, the airway setup becomes more controlled because both tube compression and tube displacement are being addressed within the same management strategy.
How Bite Blocks Protect Endotracheal Tubes During Ventilation
During ventilation, the endotracheal tube sits in an environment where oral pressure can change quickly. Jaw tension, reflex biting, and repeated compression can alter the tube wall enough to reduce internal diameter or disturb airflow. In patients who are lightly sedated, neurologically reactive, or intermittently agitated, that pressure may become strong enough to compromise ventilation before any external tube movement is even visible. The tube may still appear to be in place while airflow through it is already being restricted.
Bite Blocks protect the tube by separating the teeth from the airway device and absorbing the force that would otherwise be directed onto the tube itself. This helps preserve lumen shape and maintain a more stable airflow pathway during ventilation. It also reduces the chance that clinicians will have to respond to avoidable tube-related obstruction, which can interrupt support and complicate an already unstable airway situation. In practice, tube protection is not only about preserving the device. It is about preserving the conditions required for reliable ventilation.
Why Bite Blocks Are Critical in Preventing Airway Obstruction
Airway obstruction can develop quickly when a tube is compressed at the oral level because the ventilator continues to deliver support into a pathway that has suddenly changed in diameter. As resistance rises, airflow delivery becomes less efficient and the patient may begin to show higher airway pressures, reduced chest movement, or worsening oxygenation. In a setting where timing matters, that kind of mechanical obstruction can create a rapid shift in patient status without any change in the ventilator settings themselves.
Bite Blocks reduce that risk by protecting the airway lumen from bite-related narrowing. Once the tube remains open, delivered breaths are more likely to match what the ventilator is set to provide, and clinicians can interpret changes in respiratory status with fewer mechanical confounders. This matters in acute care because airway obstruction is not always caused by secretions, bronchospasm, or tube displacement alone. Oral compression can be the trigger, and when it is prevented early, the airway remains more stable and easier to manage.
How Bite Blocks Improve Patient Safety During Sedation Changes
Sedation changes often reveal how vulnerable the airway can become when the patient transitions from deeper suppression to a more responsive state. During weaning, neurological checks, or lighter sedation periods, patients may clench, bite, or react unpredictably to the presence of the tube. These responses are not minor events because they can place sudden force on the airway device at the exact time when the care team is trying to assess respiratory drive, neurological function, or readiness for further reduction in support.
Bite Blocks help make these transitions safer by preserving airway protection while the patient’s level of responsiveness changes. They reduce the likelihood that biting will become the event that interrupts ventilation or destabilizes the airway during assessment. This gives clinicians more confidence when managing sedation adjustments because the airway remains protected from one of the most immediate mechanical threats. In that setting, patient safety improves not because the response is eliminated, but because the airway is better prepared for it.
Why Endotracheal Tube Holder Stability Complements Bite Block Use
A protected tube still has to remain properly positioned. Bite Blocks address compression from inside the oral environment, but they do not control external movement caused by repositioning, patient motion, routine handling, or circuit pull. That is where an Endotracheal Tube Holder becomes equally important. If securement is weak, the airway can still become unstable through migration, rotation, or misalignment even when the tube itself is protected from biting.
Together, the two devices support different sides of the same airway problem. The Bite Block preserves the lumen, and the Endotracheal Tube Holder preserves tube position. When both functions are managed well, clinicians can maintain airflow and alignment at the same time, which creates a more stable setup during ventilation. That combined stability becomes especially valuable in patients who are difficult to manage, frequently repositioned, or moving through changing levels of sedation and interaction.
Clinical Considerations When Using Bite Blocks in Airway Management
Using Bite Blocks effectively requires more than placing them between the teeth. Fit, oral anatomy, tube position, and tissue condition all affect whether the device protects the airway without creating new issues. If the bite block is poorly positioned, it may fail to prevent tube contact or may place unwanted pressure on the gums, lips, or oral tissues. That can reduce tolerance and introduce avoidable oral complications over time.
Ongoing assessment is therefore part of proper use. Clinicians need to evaluate whether the device is still separating the teeth from the tube, whether oral tissues remain protected, and whether the airway setup continues to perform as intended during ongoing care. In airway management, a bite block works best when it is integrated into routine reassessment rather than treated as a one-time placement step. That approach supports both tube protection and patient safety across longer periods of ventilation.
Why B&B Medical Supports Reliable Bite Blocks and Airway Care
B&B Medical Technologies aligns with Bite Blocks and airway care because intubated patients depend on more than tube placement alone to remain stable. Tube protection, airflow preservation, and secure positioning all affect whether ventilation remains controlled during routine care, agitation, and sedation changes. Once one part of that setup becomes unreliable, the rest of the airway strategy becomes harder to maintain with consistency.
This is where B&B Medical fits naturally into airway management. Its airway-focused product approach supports the conditions that help ventilation remain stable at the bedside, especially where device protection and securement need to work together. In patients who require prolonged airway support, those details influence whether the team can maintain a controlled respiratory setup with fewer interruptions and fewer avoidable airway complications.
Why Bite Blocks Remain Essential in Modern Airway Management
Modern airway care includes sophisticated ventilators, monitoring systems, and sedation strategies, but mechanical threats at the patient interface still carry immediate risk. Biting remains one of those threats because it can compromise the airway at the point where airflow has the least margin for disruption. If that point is not protected, even a well-managed ventilator strategy can be undermined by a simple mechanical event—a principle that parallels considerations in Continuous vs Intermittent Nebulizer Therapy in Clinical Respiratory Care, where delivery method and consistency directly impact therapeutic effectiveness.
Bite Blocks remain essential because they solve that problem directly. They protect the tube, support more consistent airflow, and help the care team maintain a safer airway during periods when patient behavior can change rapidly. When used with stable securement and careful reassessment, they continue to serve an important role in protecting intubated patients across critical care and airway management settings, much like choosing the appropriate regimen in Continuous vs Intermittent Nebulizer Therapy in Clinical Respiratory Care ensures reliable medication delivery and patient safety over time.
Frequently Asked Questions
Bite Blocks prevent patients from biting and compressing the endotracheal tube, helping preserve airflow and airway patency.
Yes, Bite Blocks help reduce the risk of bite-related airway obstruction by protecting the tube from direct compression.
They are used in intubated patients when there is a risk of jaw clenching, agitation, reflex biting, or changes in responsiveness during ventilation.
Bite Blocks protect the tube from internal compression, while an Endotracheal Tube Holder helps maintain external tube position for more stable airway support.
They are commonly used when the patient has any risk of biting that could compromise tube patency or ventilation quality.