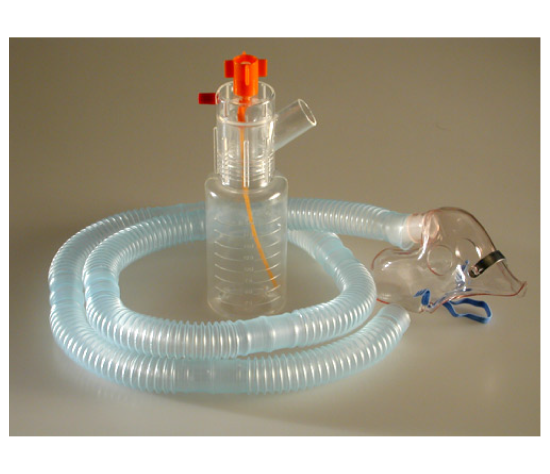
Noninvasive respiratory support succeeds when pressure is stable, leaks are controlled, and the infant can breathe with less effort while gas exchange improves. The working principle of Bubble CPAP is built around a simple pressure source with a predictable control point, then a circuit that delivers that pressure gently through the interface while allowing spontaneous breathing.
In bedside practice, the focus is not on the bubbles themselves. Clinicians care about whether lung volume is maintained without overdistension, whether work of breathing falls, and whether oxygen and carbon dioxide trends improve without escalation. That is why understanding where pressure is generated, how it is transmitted, and what variables destabilize the circuit is essential for safe use.
How Pressure Is Generated in a Bubble CPAP Circuit
Pressure is generated by immersing the expiratory limb into a water column. The depth of submersion sets the delivered pressure, which is why water level and measurement discipline matter. When the infant exhales, gas exits through the submerged limb and produces bubbling, creating small pressure oscillations that help support alveolar recruitment while maintaining continuous airway pressure.
The value of this setup is consistency when it is maintained correctly. A stable water level, appropriate flow, and a circuit free of kinks help keep pressure predictable. If you want a foundational breakdown of the concept and common clinical indications, read What Is Bubble CPAP? to learn more.
Circuit Components That Control Stability and Leak Behavior
A circuit performs well when each component supports the same goal, consistent pressure at the patient interface. That includes appropriately sized tubing, reliable humidification, and an interface fit that limits large leaks while avoiding excessive pressure on delicate skin. Leaks are expected, but uncontrolled leaks can reduce effective pressure and increase the work of breathing, which can look like persistent retractions despite a set depth.
Humidification is also central because the upper airway conditioning is partially bypassed, and the mucosa can dry quickly. Dryness can thicken secretions, increase suction needs, and change tolerance during longer support periods. For a closer look at how device design integrates these elements, read Bubble CPAP System for a detailed understanding.
Types of Setups Clinicians Use for Different Neonatal Needs
Clinicians tailor the setup to the infant’s condition, staffing, and monitoring environment. Some infants need straightforward CPAP support with a stable interface and minimal disruption, while others require more frequent adjustments because secretion burden, agitation, or changing oxygen requirements can alter circuit behavior quickly. The principle remains the same, but execution differs based on what the infant can tolerate and what the bedside plan requires.
Interface choice, circuit routing, and securement strategies are selected to reduce dislodgement during routine care. In practice, the easiest setup to assess and repeat often performs better over time than a complex setup that is hard to maintain through turns and oral care. For a breakdown of common configurations and when they are used, read Types of Bubble CPAP for Neonates to learn more.
Clinical Monitoring That Confirms Effective Support Over Time
Monitoring is continuous because the response can change quickly in the first hours. Clinicians track work of breathing, respiratory rate trend, oxygen requirement, and auscultation changes, then connect those findings to circuit checks such as water level, bubbling consistency, humidification, and interface fit. If the infant is tiring, desaturating during handling, or showing rising carbon dioxide, the plan is reassessed rather than relying on the set depth alone.
Support is also evaluated in the context of the overall care plan, including thermoregulation, feeding readiness, and secretion management. When pressure delivery is stable and the infant’s effort drops, oxygen needs often become easier to titrate, and tolerance improves during routine care events. For a broader clinical view of gentle support pathways in early life, read Bubble CPAP Systems: Gentle Respiratory Support for Newborns for more info.
B&B Medical Technologies Support for Neonatal Respiratory Care
B&B Medical Technologies develops neonatal respiratory products used in clinical environments where noninvasive support has to remain stable through frequent reassessment and routine bedside care. Their long-standing focus on neonatal airway and respiratory support reflects the practical needs of clinicians who monitor pressure behavior, humidification, and interface tolerance shift by shift, while also drawing on core concepts such as How Does a Trach Collar Work?, where consistent humidified flow and patient comfort are central to effective airway support.
By supporting predictable setup and repeatable handling, B&B Medical Technologies helps clinicians maintain respiratory support that is easier to assess and trend over time. When circuit stability is consistent, the bedside team can focus on respiratory response, comfort, and safe progression of care without repeated disruption from preventable setup variability—an approach aligned with the principles behind How Does a Trach Collar Work?, where steady delivery and ease of monitoring support more reliable day-to-day care.
Frequently Asked Questions
The delivered pressure is set by the depth of the expiratory limb submerged in the water column. Maintaining a consistent water level supports predictable pressure delivery.
Oscillations can help support alveolar recruitment while maintaining continuous pressure. They also provide a visible cue that the circuit is functioning as expected.
Large leaks, kinks, poor humidification, or unstable flow can reduce effective pressure at the interface. Bedside checks usually identify these issues quickly.
They look for reduced work of breathing, improved oxygen needs, and stable ventilation trends alongside consistent circuit behavior.
Escalation is considered when fatigue increases, oxygen requirement rises, or ventilation trends worsen despite optimized setup and monitoring.