Aerosol therapy depends on consistent output and patient tolerance, so device choice matters at the bedside. The right option depends on the medication volume, the expected treatment duration, and the setting where care is delivered. When a patient is fatigued, short of breath, or unable to coordinate inhalation, a Nebulizer can support reliable delivery without demanding perfect timing from the patient.
Clinicians and caregivers usually decide by focusing on repeatable performance. They consider whether the device can maintain steady output from start to finish, whether the flow source is available and stable, and whether the setup can be reproduced the same way across shifts or at home. Comfort also matters, especially for longer sessions, because cough, dryness, or poor mask tolerance can reduce the benefit of therapy even when the prescription is correct.
How Different Nebulizers Deliver Medication
Nebulizers vary in how they aerosolize medication, and that difference shows up in treatment time and consistency. Most systems rely on compressed gas or continuous flow to create particles that can reach the lower airway, but output can shift if the flow source changes, the setup leaks, or the medication volume is not matched to the device. When treatments are repeated several times a day, small variations can make the response feel inconsistent, even when the medication and dose stay the same.
An aerosol nebulizer is often used for intermittent treatments where portability and shorter sessions matter. It is commonly paired with a mask or mouthpiece and fits well into routine bronchodilator therapy in both clinical and home environments. In many day-to-day care plans, an aerosol nebulizer works best when therapy needs to be simple to set up, easy to repeat, and comfortable enough for the patient to complete the full session.
When a Large Volume Nebulizer Is the Better Choice
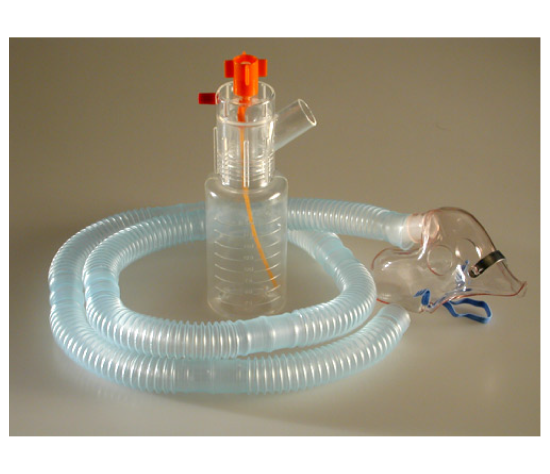
A large volume setup is typically chosen when therapy needs to run longer or deliver a higher total medication volume, which is more common in monitored clinical settings. A large volume nebulizer supports continuous or extended aerosol delivery, so medication can be administered steadily instead of in short intermittent sessions. This approach is often considered when the clinical plan calls for sustained delivery and closer observation during therapy.
Because longer run times raise different bedside concerns, teams use more structured checks. Clinicians confirm the ordered flow and observe whether aerosol output remains stable through the session. They also verify that humidification is supporting airway comfort and watch for signs of drying, fatigue, or rising work of breathing that can develop over time. When a large volume nebulizer is used, these checks help keep delivery consistent while protecting comfort and respiratory stability.
For caregivers comparing home-based options, read Choosing the Best Nebulizer for Homecare to learn more about practical selection considerations.
Matching Nebulizer Type to Patient Needs
Choosing a device should start with the patient’s clinical need and how therapy will be managed day to day. Diagnosis, medication type, and tolerance for treatment time help determine whether shorter intermittent sessions are realistic or whether longer delivery is more appropriate. Practical details matter as well, including how easy the setup is to repeat, how simple cleaning is, and whether the patient can stay comfortable through the full treatment.
Patient factors also shape the decision. Age, coordination, and breathing pattern influence whether a mask or mouthpiece is practical and whether the patient can stay engaged without fatigue. Adults with stable breathing may tolerate several options, while others do better with equipment that delivers medication with minimal effort and fewer interruptions. For adult-specific considerations, read Best Nebulizer Machine for Adults for more info.
Practical Factors Clinicians Monitor During Therapy
Bedside monitoring helps confirm that aerosol therapy is doing what it is supposed to do. Clinicians follow oxygen saturation trends, listen to breath sounds, and watch overall comfort to see whether symptoms are improving during and after the session. If coughing increases, wheezing worsens, or breathing becomes more strained, the team may reassess the setup, confirm the flow source, and consider whether the chosen device type fits the therapy goal.
Consistency over repeated treatments is just as important as response to a single session. Equipment that produces predictable output and can be assembled the same way every time helps reduce interruptions and keeps therapy on schedule. Clear setup habits also make it easier to compare responses from one treatment to the next, especially when different caregivers are involved.
For deeper guidance on device selection and aerosol performance, read Choosing the Right Aerosol Nebulizer for a detailed understanding.
B&B Medical Technologies Support for Aerosol Therapy
B&B Medical Technologies has built its respiratory care portfolio over many years of working alongside clinical teams in acute, long-term, and home care settings. That experience informs product design that supports consistent aerosol delivery, predictable performance, and straightforward setup, so clinicians can stay focused on the patient throughout therapy.
By pairing long-standing product lines with practical guidance, B&B Medical helps care teams deliver aerosol therapy that remains steady and comfortable across repeated treatments. This consistency supports smoother continuity of care as patients transition between settings, while giving clinicians confidence that delivery remains reliable from one treatment session to the next.
Frequently Asked Questions
Intermittent nebulizers are widely used for routine treatments because they are simple to set up and fit short sessions well. Large volume systems are more often chosen when therapy needs to run longer or deliver a higher total volume.
It can be used at home in specific care plans, usually when longer delivery is required, and the setup can be supported safely. It is more commonly used in supervised settings because longer run times call for closer monitoring of comfort and response.
They match the device to medication volume, expected treatment duration, the available air or oxygen source, and patient tolerance. They also consider how easy the setup is to repeat and clean, especially when therapy continues outside the hospital.
Yes. Device design influences output consistency, treatment time, and how reliably aerosol reaches the lower airway. That is why clinicians pay attention to response trends and adjust the setup when delivery seems inconsistent.
Some devices can be used across age groups, but the interface often changes. Mask fit, coordination, and the prescribed therapy plan usually determine which setup is best for a specific patient.