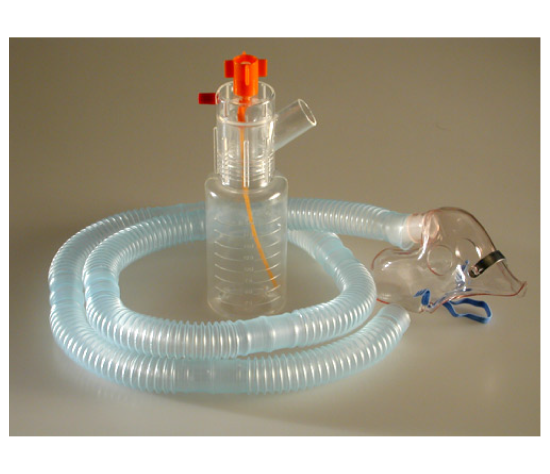
Ipratropium bromide is sometimes delivered by nebulization when clinicians want bronchodilator support without relying on patient technique. In early life, the decision is driven by diagnosis and bedside response, not by convenience, because infants have narrow airways, variable work of breathing, and limited reserve when symptoms escalate. When therapy is ordered, the priority becomes consistent delivery, careful monitoring during the session, and a plan for reassessment.
A Nebulizer for Infants is used because medication can be delivered during normal breathing with a properly fitted interface and a stable setup. Even then, tolerance and technique still matter. Mask seal, crying, fatigue, and secretion burden can all change how much medication is actually delivered. That is why clinicians watch the patient’s pattern of breathing, auscultation changes, and oxygen trend rather than assuming the ordered therapy equals the delivered dose.
When Ipratropium Is Considered and What It Targets
Ipratropium is an anticholinergic bronchodilator that reduces bronchoconstriction by blocking muscarinic receptors in the airway. In pediatric care, it is most often discussed in the context of acute bronchospasm and wheeze, where clinicians are also assessing response to other bronchodilators. In some emergency and inpatient pathways, it may be paired with short-acting beta agonists for short-term support during an exacerbation, based on clinician judgment and protocol.
Because infant respiratory presentations vary widely, treatment selection should be clinician-directed. The same symptom, such as wheeze, can reflect very different physiology depending on age, infection status, and baseline airway reactivity. For families who are trying to understand how aerosol therapy may fit into early respiratory care, read How Do Nebulizers Benefit Newborns with Respiratory Issues? for more info.
How a Nebulizer Setup Affects Delivery in Infants
A Nebulizer delivers aerosol over minutes, which reduces reliance on coordinated inhalation, but it does not remove the need for a controlled setup. Mask fit and seal are often the largest determinants of effective delivery. Leaks, frequent mask lifting, or a mask that rides up toward the eyes can reduce dose delivery and increase distress, which further disrupts breathing patterns.
Clinicians also consider flow source, treatment time, and whether secretions and humidity are influencing tolerance. If the infant is crying throughout the session, aerosol delivery becomes less predictable, and fatigue can increase the work of breathing. These are practical reasons that bedside monitoring remains central during aerosol therapy rather than treating a session as a passive process.
Nebulizer for Infants Monitoring During and After Treatment
Monitoring is based on the infant’s work of breathing, oxygen requirement, heart rate trend, and clinical response during the treatment window. Respiratory therapists and clinicians reassess breath sounds, retractions, and overall comfort to determine whether the therapy is helping or whether the plan needs adjustment. In higher acuity settings, monitoring also includes watching for rapid fatigue or deteriorating patterns during handling.
Parents and caregivers should not be asked to make therapy decisions alone. If home treatments are prescribed, clinicians typically provide specific guidance on what improvement should look like, what changes require escalation, and when the infant should be evaluated urgently. For a focused age scenario, many caregivers ask about, read Is Nebulizer Safe for 2-Month-Old Baby? for a detailed understanding.
Safety Questions Around Nebulizer for Newborns
Respiratory support in the first weeks of life should always be guided by a neonatal clinician, because newborns can decompensate quickly and symptoms may not track neatly with severity. A Nebulizer for Newborns may be used in hospital pathways when aerosol therapy is clinically indicated, and monitoring is available. Outside of supervised care, the concern is not only medication selection, but whether the newborn is stable enough for home delivery and whether the caregiver can recognize deterioration early.
When families ask whether aerosol therapy is appropriate in newborns, the answer depends on diagnosis, prescribed medication, and the monitoring plan. Clinicians also consider hydration and secretion behavior, because thickened secretions and suctioning needs can change quickly in this age group. For a broader context on early age safety questions, read Are Nebulizers Safe for Newborns? to learn more.
B&B Medical Technologies Support for Infant Aerosol Therapy Workflows
B&B Medical Technologies has spent years developing respiratory care products that support consistent aerosol delivery across hospital, alternate site, and homecare environments. That experience shapes products designed for predictable performance during repeated use, where small variations in setup, fit, or handling can meaningfully affect infant tolerance and clinical response. In early life care, reliability matters because clinicians depend on stable delivery to assess response accurately and adjust therapy without added uncertainty—an approach reflected across the portfolio, including B&B Medical Technologies: Et Tube Securement Devices, where secure positioning and consistent fit are essential to maintaining airway stability.
By emphasizing durable design, clear assembly, and compatibility with established care routines, B&B Medical Technologies supports clinicians who manage infant aerosol therapy day after day. This approach helps maintain consistency between treatments, supports clearer clinical assessment, and allows care decisions to be guided by observed response rather than variability in equipment performance, while also aligning with solutions like B&B Medical Technologies: Et Tube Securement Devices that reinforce dependable, repeatable care practices.
Frequently Asked Questions
No. It is considered for specific situations based on clinician assessment, suspected bronchospasm, and response to the overall treatment plan.
A poor seal reduces delivery and increases distress. When distress rises, breathing patterns change, and treatments become less predictable.
Clinicians usually advise watching work of breathing, feeding tolerance, color, and oxygen saturation if prescribed. Any worsening effort, lethargy, or poor intake warrants urgent reassessment.
Yes. Distress and prolonged crying can increase fatigue, which is why monitoring during the session and reassessment after are important.
Follow-up depends on diagnosis and setting. Clinicians often reassess response within the same visit or within a short window to confirm the plan is working.