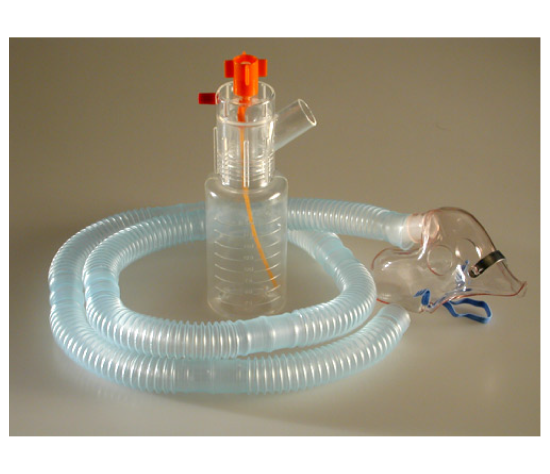
A tracheostomy changes how air enters the airway, so oxygen delivery and humidification have to be provided in a way that supports secretion control and patient comfort. A Trach collar is used to deliver oxygen, blended air, and humidification directly at the tracheostomy site, helping maintain airway moisture and reduce the drying that can increase secretion thickness and coughing.
How well the setup works depends on practical bedside factors. Flow rate, humidification performance, tubing routing, and patient tolerance all influence whether delivery stays consistent through routine care. Clinicians also reassess frequently because secretions, work of breathing, and oxygen requirement can shift during the day.
What a Trach Collar Delivers and Why Humidification Matters
A trach collar is designed to provide oxygen and humidification at the tracheostomy opening using a mask-style interface and a tubing connection to a flow source. Humidification matters because the upper airway no longer conditions inspired gas in the usual way. Without adequate humidity, secretions can become drier and more tenacious, which increases suction needs and can raise the patient’s work of breathing.
Clinicians look at the patient’s secretion behavior and comfort alongside equipment checks such as water level in the humidifier, temperature, and visible condensation patterns in the tubing. For a broader look at collar options and common care pathways, read Tracheostomy Collars to learn more.
When a Tracheostomy Tube Holder Supports Stability During Collar Use
During collar therapy, movement at the trach site can disrupt comfort and can make oxygen delivery feel inconsistent, especially when tubing pulls or the patient changes position. A Tracheostomy Tube Holder supports stable positioning of the tracheostomy tube, which helps reduce unnecessary motion at the stoma and limits irritation during routine care.
Clinicians also use securement checks to reduce avoidable events during suctioning, dressing changes, and repositioning. When a Tracheostomy Tube Holder is properly fitted and reassessed, collar delivery is easier to maintain because the interface and tubing are less likely to shift the tube during normal activity.
Set Up Choices That Improve Comfort and Delivery Consistency
Setup begins with the basics, correct interface fit, appropriate tubing length, and routing that reduces tugging. A collar that sits too high, leaks excessively, or presses on sensitive areas can increase discomfort and reduce tolerance, which often shows up as restlessness and more frequent handling. Tubing routed with slack and secured away from sharp edges reduces pull at the trach site and helps keep delivery stable.
Humidification should match the care plan, especially for patients with thicker secretions or frequent suctioning needs. Clinicians confirm flow settings, watch for signs of drying, and adjust the setup so humidity remains consistent during longer use periods.
Clinical Monitoring That Confirms the Therapy Is Working
Clinicians monitor oxygen saturation trends, respiratory rate, work of breathing, and patient comfort to confirm the collar plan is supporting stable breathing. They reassess breath sounds and secretion behavior, then connect those findings to equipment checks such as humidifier performance and tubing patency. If coughing increases, secretions thicken, or oxygen needs rise, the plan is reassessed rather than assuming the setup is unchanged.
Comfort is also a safety signal. When a patient cannot tolerate the collar, clinicians consider whether the flow is adequate, whether humidity is sufficient, and whether securement or tubing pull is contributing to distress. For a deeper clinical context on comfort-focused collar approaches, read Innovative Trach Collars: Enhancing Comfort and Respiratory Efficiency for a detailed understanding.
B&B Medical Technologies Support for Tracheostomy Respiratory Workflows
B&B Medical Technologies develops respiratory care products used in settings where tracheostomy support has to remain consistent through routine suctioning, repositioning, and daily hygiene. That experience informs designs and workflows that prioritize stable delivery, repeatable setup habits, and quick reassessment during care events, while also reflecting awareness of related considerations such as Can Bite Blocks Damage Teeth?, where proper fit, positioning, and routine evaluation help minimize unintended complications during airway management.
By supporting predictable assembly and compatibility with established respiratory routines, B&B Medical Technologies helps clinicians maintain collar therapy that is easier to monitor and trend. When a Tracheostomy Tube Holder and collar setup remain stable through handling, clinicians can focus on secretion management, oxygen titration, and patient comfort without repeated disruption from preventable movement—an approach aligned with the same careful attention seen in Can Bite Blocks Damage Teeth?, where consistent assessment and appropriate device use support safer, more reliable care.
Frequently Asked Questions
It delivers oxygen and humidification directly at the tracheostomy site, supporting comfort and secretion control during spontaneous breathing.
Many do, because inspired gas is no longer conditioned by the upper airway. Clinicians match humidification to secretion behavior, comfort, and the care setting.
Tubing pull, leaks, or poor humidity can increase coughing, thicken secretions, and make oxygen delivery feel inconsistent. Clinicians reassess early when tolerance changes.
It is reassessed throughout the day based on oxygen trends, work of breathing, and secretion needs, and also after care events like repositioning or suctioning.
Yes, when the plan is prescribed, and caregivers are trained on equipment checks, cleaning, and when to seek help. Follow-up is important if symptoms change.