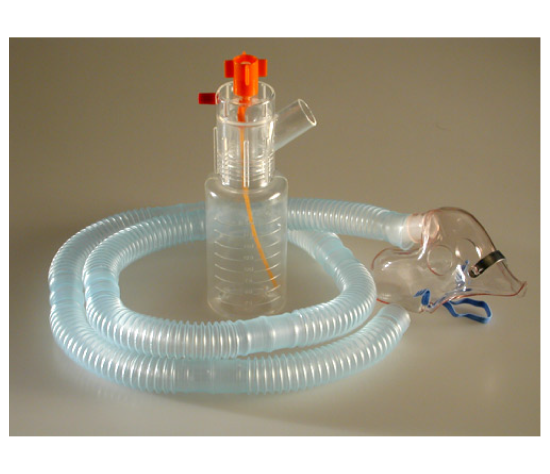
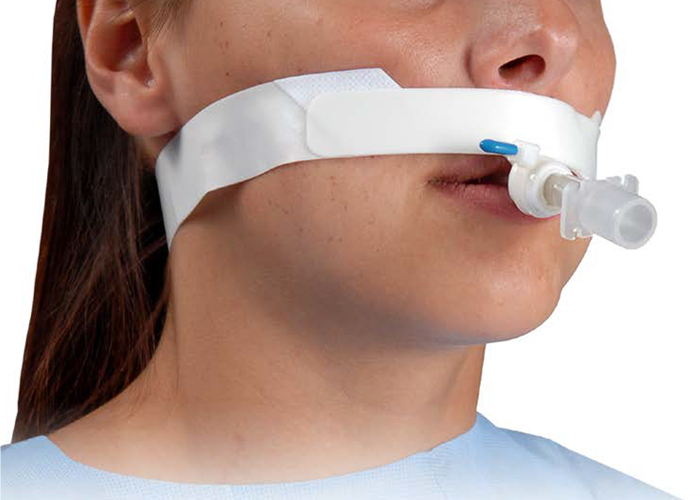
Aerosol therapy becomes clinically meaningful when delivery behavior matches airway need. In acute and critical care, the question is not simply which drug to use, but how the Nebulizer is run over time while airway resistance, work of breathing, and secretion dynamics continue to change. Continuous and intermittent delivery create different pressure, timing, and deposition patterns inside the airway. Those patterns influence how bronchodilators act, how quickly inflammation is brought under control, and how reliably oxygenation improves under therapy.
Continuous and intermittent Nebulizer strategies, therefore, represent two different ways of managing the same airway problem. One maintains a steady medication presence to stabilize a reactive airway that fluctuates minute to minute. The other introduces medication in defined intervals so clinicians can observe response, titrate dosing, and avoid unnecessary exposure. Selecting between them depends on how unstable the airway is, how quickly symptoms recur between doses, and how much control the care team needs over the treatment window.
How Continuous Nebulizer Therapy Stabilizes a Reactive Airway
Continuous Nebulizer therapy is used when the airway cannot maintain stability between doses. In conditions like severe bronchospasm or ongoing inflammation, patients often show a short-lived response after each treatment, followed by a quick return of resistance and work of breathing. That cycle makes control difficult because the airway keeps shifting between improvement and decline. Continuous delivery changes that pattern by maintaining a steady presence of medication within the airway, allowing bronchodilation and anti-inflammatory effects to build and hold rather than fade between doses.
At the bedside, this steady input makes patient response easier to read. When medication delivery remains consistent, changes in respiratory pattern, airway pressure, or oxygenation are more likely tied to the patient’s condition rather than gaps in therapy. This helps clinicians judge whether the airway is truly improving or still unstable, which is critical in patients who cannot yet tolerate breaks in treatment without losing control over airflow.
How Intermittent Nebulizer Therapy Supports Controlled Dosing and Assessment
Intermittent Nebulizer therapy is used when the airway can hold its response for a meaningful period after treatment. Instead of maintaining a constant aerosol presence, the medication is delivered in defined sessions and then allowed to wear off while the care team observes what happens next. That structure is useful because it shows whether the airway remains open, how long bronchodilation is maintained, and whether symptoms return in a gradual way or begin to recur quickly. In clinical respiratory care, those intervals are not empty space between treatments. They are part of the assessment.
This makes intermittent therapy valuable when clinicians need to titrate support with more precision. Frequency, dose, and medication choice can all be adjusted based on how the patient behaves after each session rather than on continuous exposure alone. It also helps limit unnecessary cumulative drug delivery in patients who do not need sustained aerosol input. In practice, intermittent therapy supports a more measured treatment rhythm in which response, duration, and recurrence all guide the next respiratory care decision.
Key Differences in Airway Behavior Under Continuous vs Intermittent Use
The difference between continuous and intermittent Nebulizer therapy becomes clear when airway behavior is observed across time instead of during the treatment alone. With continuous delivery, medication input stays active, so the airway is less likely to move through repeated narrowing and reopening cycles. This can reduce rebound bronchospasm, limit swings in airflow resistance, and create a more even treatment background in patients whose symptoms change quickly. The airway tends to remain under steadier therapeutic influence.
With intermittent delivery, the airway has to sustain its response after each treatment session ends. That gives clinicians a clearer view of how long the effect lasts and how dependent the patient remains on repeated aerosol support. Some patients hold improvement well and move toward wider spacing between doses, while others begin to tighten again as the interval progresses. That difference guides treatment planning because it shows whether the airway is moving toward stability or still requires continuous pharmacologic support to remain controlled.
Clinical Factors That Guide Nebulizer Therapy Selection
Selecting the right Nebulizer strategy starts with understanding how unstable the airway is at that moment. A patient with severe wheeze, rising work of breathing, recurrent tightening between doses, or persistent difficulty moving air often benefits from continuous therapy because the airway is not yet able to hold its response. A patient who maintains better airflow and oxygenation after each treatment may be ready for intermittent delivery, where spacing between doses becomes part of the management plan rather than a point of risk.
The decision also depends on how the therapy fits the broader respiratory picture. Medication class, expected duration of action, secretion burden, tolerance to aerosol delivery, and the goals of care all influence which method makes more sense. In many cases, treatment begins with continuous delivery to regain airway control and later shifts toward intermittent sessions as stability improves. That transition reflects improving airway behavior and a reduced need for constant pharmacologic support.
How Nebulizer Performance Influences Deposition and Outcomes
A Nebulizer only performs well when aerosol output remains consistent enough to produce predictable deposition in the airway. Particle size, flow source, residual volume, humidity, and interface conditions all influence whether medication reaches the lower respiratory tract or is lost before it can contribute to therapy. In clinical care, this affects more than efficiency. If output changes from one treatment to the next, the patient may appear to respond differently even when the medication plan itself has not changed.
Stable performance gives clinicians a clearer basis for interpreting the outcome of therapy. When deposition remains more consistent, changes in wheeze burden, airway pressure, oxygen need, or work of breathing can be tied more confidently to patient response rather than to delivery variation. That makes both continuous and intermittent treatment easier to manage because the care team is adjusting therapy against a steadier delivery platform instead of trying to compensate for aerosol inconsistency.
Why B&B Medical Supports Reliable Nebulizer Therapy in Clinical Care
B&B Medical Technologies supports respiratory care with a long-standing focus on airway management, delivery consistency, and device performance in active clinical settings. In aerosol therapy, the quality of treatment depends on how reliably medication can move from the device to the airway under the pressures of routine care, changing respiratory status, and different support environments. A Nebulizer is only as useful as the consistency it maintains during treatment, because clinicians need to know that changes in patient response reflect airway behavior rather than preventable variation in delivery.
That is where B&B Medical brings depth to Nebulizer care. Its respiratory product focus supports treatment setups that are easier to manage with confidence across both continuous and intermittent therapy plans. By emphasizing dependable performance and compatibility within broader respiratory care workflows, B&B Medical helps clinicians maintain a steadier treatment environment, make more accurate adjustments, and manage inhaled therapy with greater control when patient status remains variable.
Why Nebulizer Therapy Remains Central in Respiratory Management
A Nebulizer remains central to respiratory management because it allows medication to be delivered directly to the airway in a form that can be adjusted to fit different phases of illness. Continuous therapy supports stabilization when airway behavior is highly reactive, while intermittent therapy supports controlled dosing when the patient can hold improvement between sessions. Both approaches remain clinically useful because respiratory care is rarely static, highlighting the same careful consideration reflected in How to Choose the Best Nebulizer for Infants?, where selecting the right device involves matching equipment performance to patient size, tolerance, and clinical goals.
This adaptability gives clinicians a way to match treatment timing to airway behavior rather than forcing the same pattern across every stage of care. When the therapy mode, delivery quality, and patient response are interpreted together, a Nebulizer becomes more than a medication device. It becomes part of how clinicians evaluate progression, judge response, and move respiratory support forward with greater precision—mirroring the thoughtful decision-making emphasized in How to Choose the Best Nebulizer for Infants?, where proper device selection directly supports safer, more effective therapy.
Frequently Asked Questions
Continuous therapy delivers medication without interruption, while intermittent therapy provides it in scheduled sessions with observation between doses.
It is used when the airway does not maintain its response between treatments and requires sustained medication exposure.
Yes, it supports controlled dosing and allows clinicians to evaluate how the airway responds over time.
They assess airway stability, response pattern, oxygen needs, and how quickly symptoms return between treatments.
Yes, consistent aerosol delivery supports predictable deposition and more reliable clinical response.