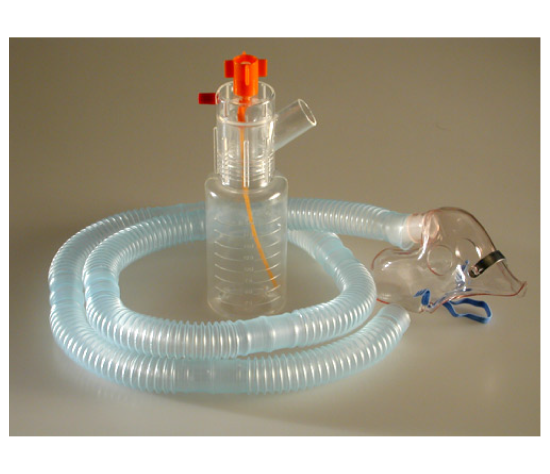
Inhaled medications succeed or fail based on dose placement and consistency. Aerosol Therapy refers to the delivery of medication as airborne particles, but the real-world outcome depends on practical variables clinicians see every day, including breathing pattern, inspiratory flow, airway obstruction, and interface leak.
When the same medication produces different results, the delivery method is often the reason. Clinicians sort options by how technique-dependent they are, how well they perform during rapid or shallow breathing, and what airway region is most likely to receive the dose. A clear understanding of Aerosol Therapy Types helps teams choose a method that is reliable at the bedside, then troubleshoot quickly when the response is less than expected.
What Clinicians Mean by Inhalation Treatment
Inhalation treatment turns a liquid or metered medication into small particles that can be breathed into the airways. The value is direct airway delivery, which is often preferred when symptoms are coming from bronchospasm, airway inflammation, or mucus that is sitting in the bronchial tree and needs targeted support.
How much medication reaches the lungs depends on both the aerosol and the patient’s breathing. Fast, shallow breaths can limit lower-airway delivery, and even a small leak at the mask or mouthpiece can send part of the dose into the room. Because these issues show up frequently in real care, clinicians treat device choice and interface fit as part of the plan, then reassess response with those delivery conditions in mind.
The Most Common Delivery Categories in Practice
In most hospital, clinic, and home care pathways, inhaled medications are delivered through three main device categories. Each category tends to fall short for a predictable reason in day-to-day use, so understanding the common failure points helps clinicians improve the delivered dose before changing the medication plan.
- Nebulizer-Based Delivery (Jet, Mesh, or Ultrasonic)
Nebulizers generate aerosol over minutes of relaxed breathing, which supports delivery when coordination is poor or the work of breathing is high. Jet nebulizers use compressed gas flow, while vibrating mesh devices generate aerosol through a perforated membrane and may reduce medication waste in certain setups. Ultrasonic systems use high-frequency vibration, and compatibility can vary by medication type. - Metered-Dose Inhalers (MDIs), Often With a Spacer or Valved Holding Chamber
MDIs deliver a measured dose quickly, but effectiveness depends on timing. Spacers and holding chambers reduce oropharyngeal deposition and make delivery more repeatable, especially in pediatrics or when the patient cannot coordinate actuation and inhalation precisely. - Dry Powder Inhalers (DPIs)
DPIs are breath-actuated and depend on sufficient inspiratory flow to disperse powder. They can be efficient when the patient can generate the required flow, but performance may decline during acute distress, fatigue, or severe obstruction.
For a deeper foundation on how aerosol generation and airway deposition guide real device selection, read Aerosol Therapy: A Comprehensive Guide to Inhalation Treatment for a more in-depth explanation.
How Clinicians Choose the Right Method
Clinicians start by carefully assessing how the patient is breathing in real time, paying attention to the work of breathing, rhythm, and the patient’s ability to coordinate a steady inhalation. When breathing becomes rapid, shallow, or irregular, delivery methods that depend on precise timing or strong inspiratory effort may fail to deliver the full dose, even when the medication choice is appropriate. In these situations, approaches that allow a longer delivery window and rely less on coordination tend to provide more consistent airway exposure.
Once breathing mechanics are understood, clinicians align the delivery method with both the medication plan and the care environment. This includes confirming oxygen flow requirements, determining whether humidification is part of the respiratory pathway, and ensuring the interface can remain secure during coughing, movement, or repositioning. These practical considerations directly influence whether the intended dose is delivered reliably from one treatment to the next, which ultimately shapes clinical response.
Practical Checks That Improve Delivered Dose
Many delivery problems come from small setup details that are easy to overlook during busy care. A mask that leaks, a mouthpiece that is poorly positioned, or a patient who cannot maintain calm inhalation can reduce airway deposition more than clinicians expect. Upright positioning, a stable seal, and completing the full dose volume tend to improve results more reliably than adding extra treatments.
Device hygiene and routine maintenance also influence output and safety. Residue and trapped moisture can change output and raise contamination risk, which is why cleaning and drying should follow the instructions for use, and standardized replacement intervals should be routine in clinical workflows. When the main question is device selection and performance differences, read Choosing the Right Aerosol Nebulizer for Respiratory Therapy for a more detailed comparison.
B&B Medical Technologies and Respiratory Aerosol Delivery
B&B Medical Technologies has supported respiratory care for decades with a product line built around practical airway delivery needs, including nebulizer systems, aerosol accessories, and components that fit common clinical workflows. In Aerosol Therapy, that experience shows up in details that affect delivered dose, such as stable aerosol output, dependable connections, and interface options that remain comfortable during coughing, higher work of breathing, and routine handling at the bedside.
For hospitals and providers standardizing aerosol delivery, B&B Medical Technologies offers long-standing product offerings designed to behave consistently as a set, which helps staff train faster and troubleshoot with the same checkpoints across shifts. That consistency supports clearer documentation of delivery conditions and more reliable reassessment, because teams can separate a device or setup issue from a true change in the patient’s respiratory status. Just as clinicians track questions like “How fast do hydrocolloid patches work on wounds?” to set expectations for healing, consistent aerosol delivery allows care teams to distinguish whether changes in patient response are due to therapy technique or the underlying condition.
Frequently Asked Questions
Most clinical settings rely on nebulizers, metered-dose inhalers, and dry powder inhalers. The best choice depends on coordination, inspiratory flow, airway obstruction, and the medication being delivered.
When breathing is rapid or coordination is limited, methods that depend on precise timing or strong inspiratory effort can underdeliver. Clinicians often favor approaches that allow a longer delivery window and do not require precise timing, but the final choice depends on diagnosis and available equipment.
The delivered dose can change with leaks, breathing pattern, and inspiratory flow requirements. If the device does not match the patient’s mechanics, airway deposition drops even when the prescription is appropriate.
Mask leaks, poor mouthpiece position, rapid shallow breathing, and stopping treatment early are common causes. Cleaning and maintenance issues can also affect output and consistency.
They reassess work of breathing, wheeze, airflow, oxygen need, and patient comfort, then compare trends after a properly delivered dose. Response assessment should follow a documented reassessment plan tied to the condition being treated.