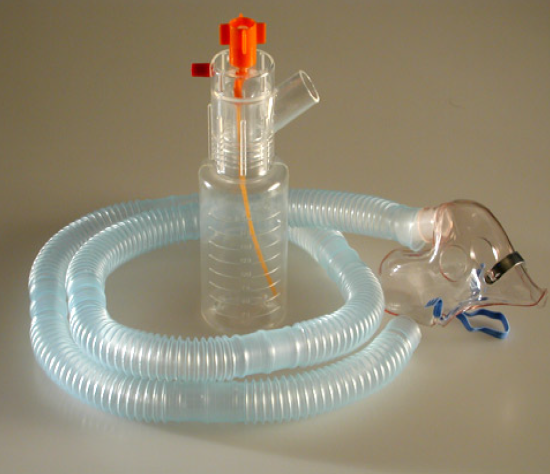
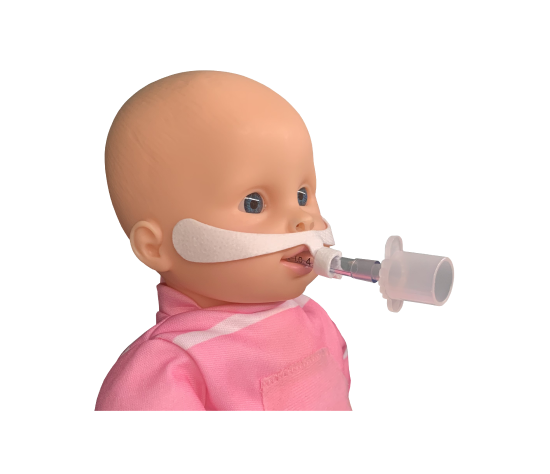
A tracheostomy changes where air enters the airway, which also changes how oxygen, humidity, and secretion clearance need to be managed. A Trach Collar is commonly used to deliver humidified oxygen over a tracheostomy, helping clinicians support oxygenation while keeping airflow comfortable and secretion management more predictable. It is often selected when a patient is breathing spontaneously, and the goal is stable support rather than mechanical ventilation.
In real bedside use, the decision is rarely only about oxygen percentage. Clinicians also consider secretion thickness, cough effectiveness, comfort, and how quickly airway dryness can lead to plugging or increased work of breathing. When the setup is matched well to the patient, it supports steadier breathing and reduces interruptions caused by dry mucosa, crusting, and frequent circuit adjustments.
What Is a Trach Collar Used For?
The most direct use is to provide oxygen with humidification to a patient who is breathing through a tracheostomy. Humidity matters because the upper airway normally warms and moistens inhaled air, and that function is bypassed after a trach. When humidity is inadequate, secretions can thicken, suction needs may increase, and the risk of mucus plugging rises.
Clinicians also use a collar setup as part of weaning and ongoing airway management. It allows oxygen support without introducing ventilator pressure, which helps assess spontaneous breathing endurance and tolerance. In that context, the collar becomes a practical way to support oxygenation while monitoring how the patient handles secretion clearance, cough strength, and overall respiratory effort.
Humidification and Secretion Management in Tracheostomy Care
Humidification is not an optional comfort feature in tracheostomy care. It is a control point that influences secretion behavior and airway patency, especially during long periods of spontaneous breathing. When secretions stay hydrated, suctioning is often less traumatic, and airway resistance is less likely to change abruptly between assessments.
Bedside practice usually includes watching secretion volume and texture, listening for new coarse sounds, and reassessing the need for suctioning frequency. Small changes in humidity delivery can show up quickly as thicker secretions or more frequent desaturation during care events. For a broader background on collar options and common setups, read Tracheostomy Collars to learn more.
Set Up Choices That Affect Comfort and Delivery Consistency
A collar setup works best when delivery remains stable during routine care. Fit around the stoma area, tubing routing, and how the humidifier connects all influence whether humidity and oxygen reach the airway consistently. Leaks around the collar are expected, but the goal is to avoid a setup that shifts constantly with movement or pulls during repositioning.
Clinicians often make adjustments based on patient comfort and observation rather than numbers alone. If the patient shows increased work of breathing during turns or becomes more distressed during suctioning, the setup is reassessed for dryness, circuit pull, or inadequate humidification. For selection guidance that connects collar type to patient needs, read Choosing the Right Trach Collar for Tracheostomy Patients for a detailed understanding.
Clinical Monitoring While Using a Trach Collar
Monitoring focuses on more than oxygen saturation. Respiratory therapists and bedside clinicians track respiratory rate, work of breathing, breath sounds, and trends during routine activities such as oral care, suctioning, and mobility. Changes that appear during care events can be early indicators that humidity delivery is insufficient or secretions are becoming harder to clear.
Clinicians also pay attention to alarm patterns and the patient’s overall tolerance over time. If oxygen needs rise, secretions thicken, or fatigue develops, the collar plan is reassessed, and escalation pathways are considered. For practical ideas that connect comfort and delivery performance, read Innovative Trach Collars Comfort and Respiratory Efficiency for more info.
Homecare and Alternate Site Considerations for Trach Collars
In home care and alternate site settings, collar use often needs to be reliable with fewer hands-on resources. That places more emphasis on stable humidification, straightforward setup, and repeatable daily checks. Care plans usually include specific guidance on suction frequency, hydration, and signs that warrant escalation, because small changes can progress quickly in a tracheostomy patient.
Securement and device stability also matter in these settings, especially when caregivers are managing movement, sleep positioning, and daily hygiene. Planning for tubing routing and minimizing pull reduces avoidable irritation and helps keep delivery steady. For related considerations in non-hospital care environments, read Tracheostomy Tube Holders Homecare and Alternate Site Settings to learn more.
B&B Medical Technologies Support for Tracheostomy Respiratory Care
B&B Medical Technologies develops respiratory care products with a clear understanding of how tracheostomy support is managed across the full continuum of care. In acute units, alternate site settings, and home care environments, clinicians and caregivers rely on equipment that delivers humidification and oxygen consistently while allowing for frequent inspection and adjustment during routine care. That long-term clinical exposure informs product design focused on stable delivery, patient tolerance, and compatibility with real bedside workflows.
By prioritizing predictable performance and repeatable setup, B&B Medical Technologies supports tracheostomy care that remains steady through daily handling, mobility, and hygiene. When devices behave consistently, clinicians can track respiratory status more accurately, manage secretions with greater confidence, and address subtle changes early, before they escalate into avoidable complications.
Frequently Asked Questions
A collar delivers humidified oxygen without ventilator pressure support. It is used when the patient is breathing spontaneously and needs oxygen and humidity.
Yes. It is commonly used during weaning and after liberation to support oxygenation and humidity while monitoring endurance and secretion clearance.
The upper airway no longer warms and humidifies inhaled air. Without adequate humidity, secretions can thicken and increase the risk of plugging.
Clinicians monitor work of breathing, breath sounds, secretion behavior, and oxygen trends during routine care events. Changes in tolerance often guide reassessment.
Reassess when oxygen need rises, fatigue increases, or secretions become harder to clear. Escalation is considered when stability cannot be maintained with noninvasive support.
Fit, tubing routing, and humidifier connection all influence stability. A setup that pulls or shifts often leads to discomfort and less consistent delivery.