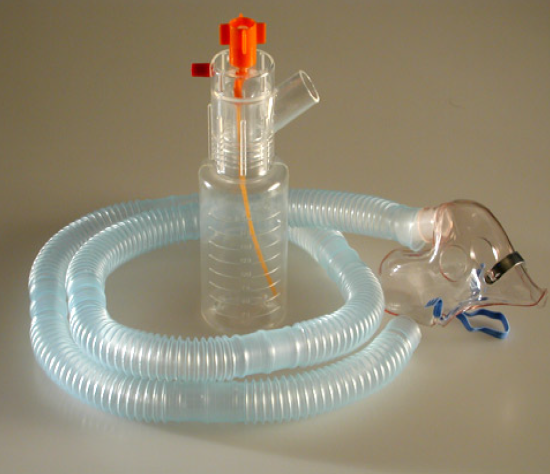
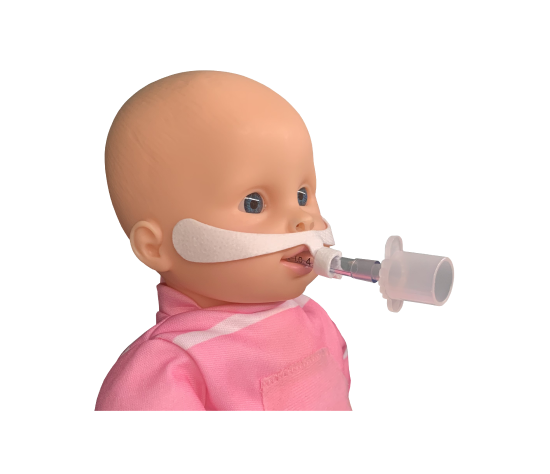
When clinicians discuss an age limit for Bubble CPAP, they are usually asking whether stable pressure delivery and a clear physiologic response are realistic for that patient. NICU clinicians and respiratory therapists focus on whether gentle distending pressure can keep lung volume stable while the infant continues to breathe spontaneously. The question becomes practical and specific, including whether the interface seals well, whether breathing effort improves after initiation, and whether oxygen needs trend in the right direction.
For clinical planning, bubble-based CPAP is used most often in premature and newborn infants because it matches how immature lungs lose volume between breaths. Even so, the Bubble CPAP age limit is better treated as a clinical window guided by fit and response rather than a fixed cutoff. This framing helps NICU clinicians apply support earlier when it is likely to help and reassess quickly when the situation is moving in the other direction.
Why Early Infancy Is the Primary Use Case for Bubble CPAP
Immature lungs tend to collapse at the end of exhalation, and that collapse raises the work of breathing and oxygen demand. Continuous distending pressure helps maintain functional residual capacity, so each breath starts from a more stable lung volume. When the infant is breathing but struggling to keep airways open, this support can reduce retractions and stabilize oxygenation without moving immediately to invasive ventilation.
This is also why selection is tightly linked to interface fit. If prongs or mask sizing are off, leak increases, pressure delivery becomes inconsistent, and the clinical response becomes harder to interpret. For foundational context on setup and mechanism, read What Is Bubble CPAP? A Complete Guide to learn more.
Clinical Criteria That Guide Bubble Support Beyond Age
NICU clinicians and respiratory therapists usually track response in the first hours and then through routine care cycles. A useful response often looks like lower work of breathing, steadier saturations at the same or lower oxygen, and fewer apnea or desaturation events as the lungs stay recruited. Clinicians also watch for the opposite pattern, including rising oxygen need, persistent tachypnea with fatigue, or pressure requirements that keep climbing.
These signals are also interpreted alongside comorbid factors. Infants with evolving respiratory distress, sepsis physiology, or airway obstruction may not respond the same way, even at the same gestational age. For a deeper discussion of why this support can be a bridge in early care, read How Bubble CPAP is a Noninvasive Lifeline for Infants for a detailed understanding.
When to Reassess, Wean, or Escalate Bubble Support
Reassessment is often triggered by trend changes rather than a single number. If retractions increase, oxygen requirement rises, or ventilation becomes less stable during handling, bedside clinicians review fit, leak, position, and whether secretions or agitation are disrupting delivery. If these factors are corrected and the response still drifts, escalation to a different mode may be clinically appropriate.
Weaning is typically considered when breathing effort remains stable, and oxygen demand stays low through routine turns, feeds, and care events. When the infant holds stability across these everyday stressors, pressure can be reduced gradually while monitoring for rebound work of breathing. For device-specific context, read B&B Bubbler – Bubble CPAP Device for more info.
B&B Medical Technologies Support for NICU Bubble Support
B&B Medical Technologies supports neonatal respiratory workflows that depend on consistent pressure delivery and repeatable bedside checks. In real unit conditions, clinicians need equipment that is straightforward to set up, easy to monitor during routine care, and reliable across shifts so trends reflect the patient rather than avoidable variation in the circuit.
Drawing on years of neonatal respiratory experience, B&B Medical Technologies builds its offerings around practical clinical use, including interface compatibility and inspection points that help respiratory therapists and bedside clinicians confirm performance quickly. When the setup remains consistent, clinicians can focus on response over time, adjust support earlier, and keep care aligned with the goals of noninvasive respiratory management.
Frequently Asked Questions
There is no universal cutoff. Clinicians base the decision on lung maturity, breathing effort, interface fit, and whether oxygen and work of breathing improve after initiation.
Yes. Some term infants use bubble-based support for a short term for transient distress when they are breathing spontaneously but working hard.
Rising oxygen need, worsening retractions, persistent tachypnea with fatigue, or instability during routine handling are common red flags. These trends trigger a fit check and a reassessment of the respiratory plan.
Weaning is considered when breathing effort and oxygen need stay stable through turns, feeds, and care events. If stability holds, pressure is reduced gradually while watching for rebound work of breathing.
Focus on whether pressure delivery is stable and whether the physiologic response is sustained over time. If fit and response remain reliable, the plan is easier to monitor and adjust.