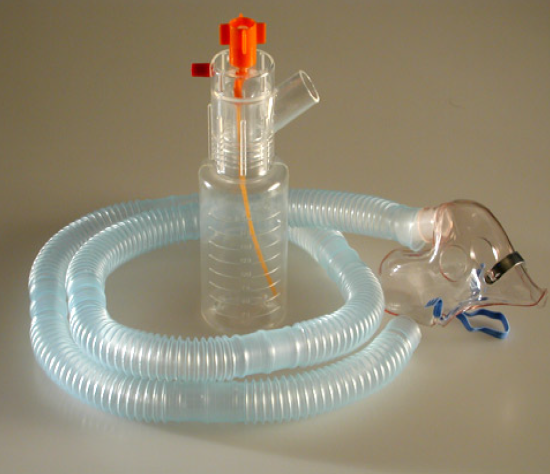
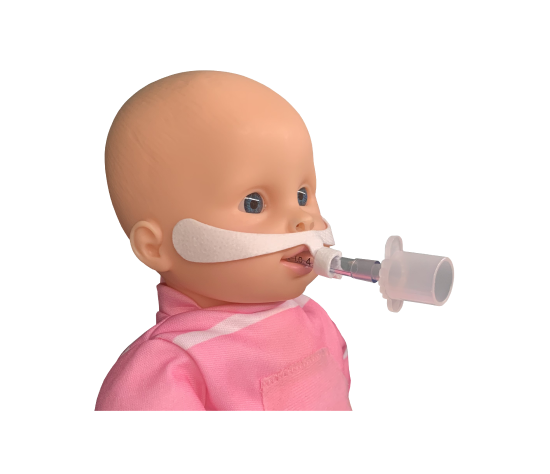
After a tracheostomy, many patients still need oxygen support, airway humidification, and a simple way to keep breathing comfortably while the upper airway is bypassed. A Trach Collar is commonly used for that purpose. It delivers oxygen and humidified flow over the tracheostomy opening, supporting patients who are breathing on their own and do not require a ventilator circuit.
In bedside care, the collar becomes part of a daily routine that includes secretion management, skin protection, and careful monitoring for increased work of breathing. The goal is to provide the prescribed oxygen concentration, keep secretions from drying, and maintain a stable respiratory pattern during rest, mobility, and recovery.
What a Trach Collar Delivers and Why It Matters
A tracheostomy collar is designed to provide oxygen, and when paired with a humidification source, it also supports moisture delivery to the lower airway. Because inhaled air no longer passes through the nose and mouth, the natural warming and humidifying effect is reduced. When humidification is insufficient, secretions often become thicker and more difficult to clear. This can lead to more frequent coughing, increased suctioning, and added discomfort for the patient.
Clinicians usually rely on a few practical checks at the bedside. They verify that the prescribed FiO₂ is reaching the patient, confirm that humidification is working as intended, and observe breathing patterns and breath sounds. Subtle changes in respiratory rate, effort, or secretion consistency often prompt a closer look at flow, humidification, or oxygen concentration.
Common Clinical Situations Where a Trach Collar Is Used
A collar is often used for patients who have a tracheostomy and are breathing spontaneously, including those transitioning from ventilator support, those on long-term oxygen therapy, and those in step-down, rehabilitation, skilled nursing, or home care settings. It can also be used during speaking valve trials or other care activities where a ventilator circuit is not in use, as long as the patient’s oxygenation and breathing pattern remain stable.
In weaning pathways, teams may use a collar to observe tolerance over longer periods while tracking oxygen needs and secretion burden. This is where consistent assessment becomes important, including pulse oximetry trends, work of breathing at rest and with activity, and the frequency of suctioning required to keep the airway clear.
For a broader clinical overview across patient types and care settings, read Tracheostomy Collars to learn more.
Trach Collar Fit, Humidification, and Comfort Checks for Safe Oxygen Delivery
Fit matters because the collar should stay in place without rubbing the skin or crowding the ties and dressing. When the collar shifts during turning or therapy, oxygen can blow away from the stoma, and moisture can collect where it becomes irritating. A simple bedside check is to confirm alignment after routine care, then watch the patient’s breathing pattern to be sure support stays consistent.
Humidification also carries the daily comfort load. Teams check the water level, confirm the humidifier is delivering warm moisture when ordered, and look for early signs of dryness such as thicker secretions, frequent coughing, or stoma irritation. When humidification is on target, secretions usually stay easier to clear, and breathing tends to look steadier through rest and activity.
If you are building a selection checklist based on diagnosis, secretion burden, and mobility needs, read Choosing the Right Trach Collar for Tracheostomy Patients for more info.
Practical Monitoring: Oxygen Response and Secretion Management
Monitoring goes beyond a single oxygen saturation reading. Teams look at trends during sleep, speaking, therapy, and ambulation because oxygen demand changes with activity. They also watch for subtle signs of fatigue, including rising respiratory rate, shallow breathing, and reduced cough effectiveness, which can appear before a clear saturation drop.
Secretion management is closely tied to oxygen and humidification delivery. If secretions become thicker, the patient may require more suctioning and may show increased work of breathing. When that pattern appears, clinicians usually reassess humidification first, then confirm oxygen concentration and flow, and finally evaluate the airway for plugging or infection signs based on the broader clinical picture.
For deeper detail on comfort-oriented design and airflow consistency, read Innovative Trach Collars Comfort and Respiratory Efficiency for a detailed understanding.
B&B Medical Technologies Support for Tracheostomy Oxygen Delivery
B&B Medical Technologies has spent decades building respiratory care products that clinicians can rely on in daily practice, from acute care to long-term and home settings. That experience shows up in designs that support stable oxygen delivery, dependable humidification performance, and straightforward bedside checks, so teams can keep care consistent even when patients are repositioned, mobilized, or transferred between units.
B&B Medical also supports standardized use by pairing long-standing product lines with practical resources that help staff set up, monitor, and troubleshoot therapy. When the same approach is used across shifts and settings, oxygen delivery stays more consistent, dryness-related secretion problems are easier to prevent, and handoffs become simpler as patients move from hospital care into rehabilitation, skilled nursing, or home care.
Frequently Asked Questions
It is used to deliver oxygen over a tracheostomy opening for patients who are breathing on their own. It is often paired with humidification to help keep secretions from drying.
No. A collar supports oxygen delivery and humidification, but it does not provide the pressure or breath delivery that a ventilator provides.
Because the upper airway is bypassed, inhaled air can be drier and cooler than normal. Humidification helps keep secretions easier to clear and reduces coughing from airway dryness.
They look at oxygen saturation trends, work of breathing, comfort, and secretion thickness. A rising respiratory rate or thicker secretions can indicate the need to reassess humidification, flow, or FiO₂.
Yes, it is commonly used in home care when patients need supplemental oxygen through a tracheostomy. Home setups still require a plan for humidification, suctioning, and monitoring based on clinician guidance.