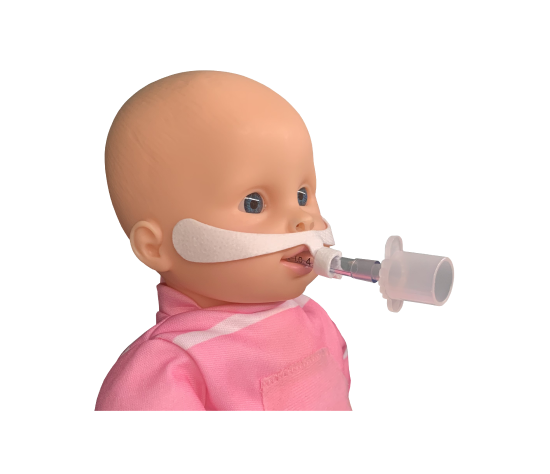
In neonatal respiratory care, clinicians focus on maintaining lung volume, easing the work of breathing, and limiting the need for invasive ventilation whenever possible. Bubble CPAP supports that goal by providing steady positive pressure through a nasal interface, helping fragile airways stay recruited while the baby continues to breathe spontaneously.
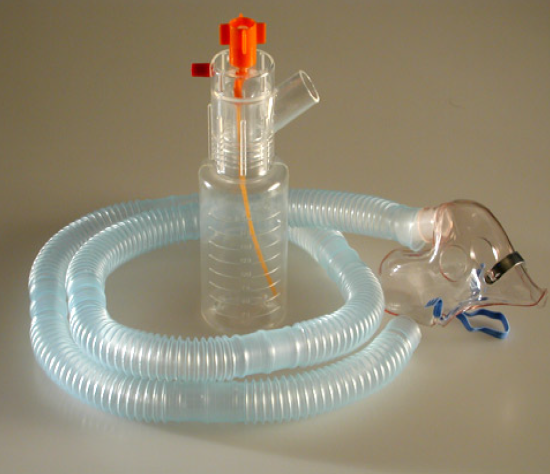
Instead of relying on a complex ventilator valve to create pressure, the system uses a water seal at the end of the expiratory limb. That water column acts like a pressure regulator. It also produces visible bubbling that helps teams confirm flow and stability at the bedside.
Bubble CPAP: What Creates the Pressure?
Pressure in a bubble setup comes from the water seal depth at the end of the expiratory limb. When the tubing is submerged to 5 cm, the circuit delivers about 5 cm H₂O, as long as flow is adequate and the nasal seal is stable. Clinicians adjust support by changing submersion depth, then reassessing comfort, work of breathing, and oxygenation to confirm the setting matches the infant’s needs.
Bubbling begins once the flow is sufficient to vent gas through the submerged tubing. The bubble pattern offers quick bedside feedback on whether flow is reaching the chamber and whether the circuit is behaving consistently. Those bubbles also create gentle pressure oscillations that can support alveolar recruitment and steadier gas exchange in some newborns, especially when leaks are controlled, and circuit resistance stays predictable.
For a broader overview, read Bubble CPAP to learn more about neonatal applications and bedside best practices.
What the Circuit Is Doing During Each Breath
During inspiration, the infant draws fresh gas from the inspiratory limb while pressure remains supported by the continuous flow in the circuit. During expiration, gas exits through the expiratory limb and vents through the water seal. Because the system maintains pressure throughout the breathing cycle, the small airways are less likely to collapse at end-expiration, which helps protect lung volume.
In day-to-day practice, stable function depends on a few basics: a comfortable interface fit, minimal leak, adequate humidification, and a flow rate that matches the baby’s needs. If the seal is poor or the flow is too low, bubbling becomes inconsistent, and the delivered pressure can drift, which may show up as increased retractions or fluctuating oxygen saturation.
The Role of Bubbling and Why It Matters Clinically
Clinicians often watch the water chamber first because it gives immediate feedback. A consistent bubble pattern usually indicates that flow is reaching the chamber and that the expiratory limb is submerged correctly. In contrast, the absent bubbling can signal a disconnection, insufficient flow, a kinked tube, or a leak large enough that gas escapes before it reaches the water seal.
The oscillations created by bubbling can also contribute to a more uniform gas distribution in the lungs. In practical terms, that can mean better maintenance of functional residual capacity and steadier work of breathing for some newborns, particularly when combined with careful positioning, suctioning when indicated, and close monitoring for leak-related instability.
For a deeper background, read What Is Bubble CPAP? A Complete Guide to learn how clinicians select candidates and plan weaning.
Key Components of a Reliable Bubble CPAP System
A consistent setup starts with the interface, the circuit, and the water seal working as one unit. A secure nasal prong fit helps limit leak without creating pressure injury. Heated humidification supports mucosal comfort and reduces secretion thickening. The expiratory limb must stay at a consistent submersion depth so the delivered pressure does not wander during routine care.
The water chamber should be positioned to prevent accidental tipping and to keep water levels stable. Teams also benefit from simple standard work: confirm submersion depth, confirm bubbling, check the nasal seal, verify humidification temperature, and document the current settings. If your team is comparing device configurations, read Bubble CPAP System for more info on setup variables and bedside checks.
Common Setup Issues and What Clinicians Check First
If a baby looks more tachypneic or begins desaturating, the quickest troubleshooting step is to confirm circuit integrity. Check for tubing kinks, loose connections, and water level changes. Then assess the interface for leak, displacement, or excessive pressure on the nares. A large leak can reduce delivered pressure even when the water depth looks correct.
If bubbling is violent, the flow may be higher than needed, or the chamber may be overfilled. If bubbling is weak or intermittent, flow may be low, the limb may not be submerged properly, or the circuit may be leaking. A structured approach helps teams correct the cause without overcorrecting the pressure support.
For a more clinical explanation of how pressure and oxygenation translate into lung mechanics, read How Does Bubble CPAP Improve Respiratory Function in Newborns? for a detailed understanding.
B&B Medical Technologies Support for Bubble-Based Therapy
B&B Medical Technologies has a long history of developing respiratory care products that are shaped by real NICU use, not just technical specifications. Its neonatal offerings are designed to deliver stable water-seal performance, consistent pressure behavior, and clear bedside feedback, so care teams can focus on the infant rather than constant circuit adjustments. This practical approach supports predictable respiratory support during repositioning, routine care, and longer periods of therapy, where small changes can otherwise affect delivered pressure.
By offering well-matched components and clear supporting resources, B&B Medical helps units standardize how Bubble CPAP is set up, monitored, and documented. A consistent Bubble CPAP System is easier for staff to learn, easier to evaluate over time, and simpler to troubleshoot when conditions change. That reliability supports smoother handoffs, clearer charting, and fewer interruptions to respiratory support during hands-on neonatal care.
Frequently Asked Questions
Pressure is set by how far the expiratory tubing sits under the water surface. If the tube is submerged to 5 cm, the circuit delivers about 5 cm H₂O, assuming the flow and nasal seal are stable.
Bubbling is a quick bedside sign that gas is reaching the water seal and venting as intended. If bubbling becomes weak or disappears, teams usually check flow, connections, kinks, and leaks around the interface.
Most NICUs start in a low-to-moderate range and then adjust based on work of breathing, oxygen needs, and comfort. The right setting depends on gestational age, lung condition, and how the infant responds over time.
Both provide continuous positive airway pressure, but a bubble setup creates pressure with a water seal instead of a ventilator valve. The bubbling can add gentle oscillations in the circuit, which may support lung recruitment in some newborns.
The most common challenges are skin irritation at the nares, pressure that drifts when leaks increase, and interruptions from kinks or water-level changes. Routine interface checks, stable chamber positioning, and consistent setup practices help prevent these issues.